ipopba - stock.adobe.com
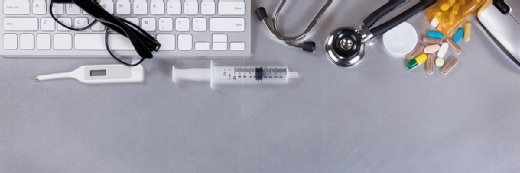
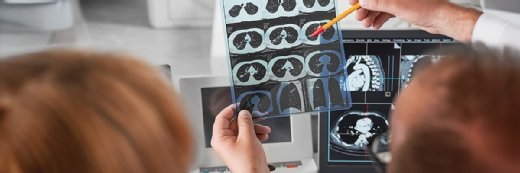
Top 10 NHS IT stories of 2023
In the year we said goodbye to NHS Digital, the NHS has made some serious strides in digitising the health service, but many challenges remain. We look back at the stories that made the headlines in 2023
It has been a hectic year for the NHS. With significant staffing challenges, a lack of beds and dwindling budgets, the NHS has faced many struggles, which could be alleviated, at least in part, with the help of technology.
2023 also saw NHS IT staple, NHS Digital, close its doors, causing redundancies and uncertainty. But despite the challenges, there has been significant progress in digitising the health service, and it is almost universally accepted that technology is the future for the health service.
In England, the NHS has hit its electronic patient records target ahead of schedule, while in Wales, the country’s version of the NHS App is making huge strides in creating a truly digital front door.
Here are Computer Weekly’s top 10 stories about the NHS in 2023.
1. Goodbye NHS Digital – a new era of NHS technology is upon us
In February 2023, the organisation which has served as the NHS technology function for more than a decade, ceased to exist. The move aimed to centralise the NHS workforce and accelerate service digitisation as part of NHS England’s change programme, but exactly what this looks like, remains to be seen.
It has long been clear that a change has been needed, with confusion around which organisation is responsible for what having perhaps contributed to a slow down in action, however, some feel that moving everything into NHS England could be a dangerous move.
2. Wales is building a dragon of an NHS app
Across the border in Wales, NHS Wales’s tech arm has been busy, creating the country’s own version of the NHS App. While at first glance, it might seem identical to the English version, the NHS Wales App is not only bilingual to account for Welsh speakers, but also has a much wider range of functionality and access, including giving patients access to all their medical information in one place, including private care, secondary care and primary care. The app will also integrate with third-party systems, such as patient portals already in place.
It’s an impressive feat, but with the next 12 months pivotal in terms of ensuring the app’s successful roll-out, how quickly it will begin to make a difference to an already strained health service remains to be seen.
3. Palantir awarded NHS FDP data contract
There has been much controversy surrounding the plans for the NHS Federated Data Platform (FDP) since its inception. The FDP aims to replace the data platform put together during the height of the Covid-19 pandemic. NHS England hopes that the ability to share real-time data about bed availability, waiting lists, staff rosters, social care places and medical supplies in a secure manner will enable a more effective and safer NHS.
The platform has been criticised by privacy campaigners, in part due to NHS England awarding the contract to run the FDP to controversial US data platform Palantir and its chequered history.
Despite the concerns, which NHS England has tried to alleviate by promising that the contract forbids Palantir to use any patient data for commercial gain, the platform will be rolled out in spring 2024.
4. NHS has the potential to get digital transformation right
In June, a report by the Health and Social Care Committee was cautiously optimistic in the NHS’s ability to succeed in its digital transformation attempt, as the latest plan, has, unlike previous attempts, clear intentions and funding to support them.
However, the NHS is still plagued by a huge digital maturity gap, with some organisations lacking even the most basic functioning IT equipment, while the majority of funding has previously been given to “exemplar” organisations, those which already have a decent level of digital maturity.
According to the committee – and probably most sensible people – the substantial variations between trusts the digital skills gap need to be addressed in order for digital transformation to succeed.
5. Government launches seven-year cyber strategy for NHS
The Department for Health and Social Care launched a new cyber security programme in March 2023, aiming to enhance cyber resilience across the NHS and social care in England over the next seven years.
This includes identifying which areas of health and social care where cyber disruption would cause the most harm to patients and support organisations to minimise cyber incidents and recovery time when they happen. The government will also complete a review of cyber security in adult social care and make updates to the Data Security and Protection Toolkit, allowing organisations to understand and own their cyber risk.
6. Government concedes it will miss 2024 e-prescribing target
Despite some positive strides forward in digitisation of the NHS, it became clear that the NHS would not meet its target of getting rid of paper prescribing by 2024. The target, which was first set back in 2019, is currently impossible, mainly due to the large variation of digital maturity in the NHS, especially when it comes to electronic prescription and medicine administration systems.
While most trusts have a system in place, functionality, age and actual use vary incredibly, and the digital infrastructure currently isn’t in place across many organisations. The government has pushed its target to 2026, which the Health and Social Care Committee’s Expert Panel believes is also unlikely to succeed. As of autumn 2023, only 3% of trusts in England have achieved paperless prescribing.
7. Kier Starmer pledges to reform the NHS through technology
While the country is currently led by a Conservative government, the Labour Party also has plans for the NHS. In a speech setting out the Party’s NHS reform plans, Labour leader Keir Starmer heralded a move from an “analogue to a digital NHS”, offering shorter waiting times, better treatment, early diagnosis and meaningful prevention.
His lofty ambitions include genomics testing for every newborn baby, centralised procurement of data systems for the NHS, and a transformation of the incentive structure for technology adoption. He also vowed to get improve GP appointment systems, bringing back the family doctor, and ensuring uptake of digital GP consultations, the latter of which only cover 1% of GP consultations, despite that fact that it is offered by 99% of GP practices.
9. Scotland launches data strategy for health and social care
Across the border, the Scottish government also made strides in its technology adoption plan, publishing its first ever data strategy for health and social care. The five-year plan is an extensive but concise document, focusing on both opportunities and challenges, and doesn’t shy away from the fact that different systems, varying levels of digital maturity and digital skills are big issues to overcome.
The aim is to transform the way people in Scotland access their personal health and care information, as well as the use of data to transform services. This includes improving standards and interoperability, data infrastructure, and data access for both individuals and health and social care staff.
9. Northern Ireland integrated care record goes live
In Northern Ireland, the country has recently deployed its first ever national care record. The care record, dubbed Encompass will be, when fully rolled out, a complete digital health and care record for every citizen in the country, linking information across different healthcare settings as well as social care.
Back in February 2023, Northern Ireland set a target of the first go-live to happen on 9 November in South Eastern Health and Social Care Trust, and low and behold, when 9 November hit, the system went live – a huge feat for the country’s health service.
10. NHS SBS to launch £1.5bn digital workplace solutions framework
This summer, NHS Shared Business Services (NHS SBS) set out plans for a new digital workplace solutions framework, aiming to provide NHS and social care with a procurement route for end-to-end IT services.
The goal is to help the NHS invest in improving NHS IT systems to make sure staff have the right technology to do their jobs, and that systems are interoperable and able to share information at the point of care.
The current framework agreement expires in August 2024, meaning NHS SBS has until then to put a new framework in place, which includes infrastructure management services, communication services, and information systems and services, among other software and products.
The aim is to publish the contract notice for the framework by the end of January 2024, a date which is looming soon after Christmas.